We build from the ground up around your workflows.
Fast deployment with minimal setup.
Hybrid rollout with a rapid MVP delivery
Let's Talk !
As healthcare providers look for ways to improve patient outcomes effectively and efficiently to promote value-based care, electronic health information sharing has emerged as a critical tool.
To coordinate care informed by detailed patient information, healthcare practitioners need the ability to work and coordinate services with other care providers; this necessitates exchanging sensitive, personal patient information. These exchanges have traditionally been made via fax or in-person deliveries, impeding clinical productivity and delaying patient care.
Electronic sharing is far more efficient. With a wealth of information essential to patient care available, disparate systems need to be able to communicate with one another. Making a synchronized healthcare system feasible, secure, and safe requires electronic health information exchanges.
Electronic Health Information Exchanges (HIE) in healthcare eliminate the burden of having to request patient information through less efficient methods. Whether from medical devices, wearables, various information systems, or patient portals, HIEs ensure that comprehensive patient data pulled from multiple sources is available to healthcare providers that need to access it, all while following applied standards of use and HIPPA guidelines.
Ultimately, this framework facilitates the seamless cooperation across a continuum of services that quality, value-based healthcare depends on.
HIEs provide a framework for authorized entities (such as providers, caregivers, insurance groups, or hospitals) to exchange protected health information necessary for patient care. With HIE interface development the transmission and storage of medical data is possible when interfaced with disparate medical data management systems and data sources, such as:
Health-based applications
Hospital Information Systems (HIS)
Electronic Health Record/Electronic Medical Record (EHR/EMR)
Laboratory Information Systems (LIS)
Practice Management Systems (PMS)
Patient Administration Systems (PAS)
Without HIEs, if a physician wanted to access patient information from an aforementioned database, they would need to access each of them separately to retrieve the relevant information. HIEs create a more centralized source of data so that care providers can simply make one request to access and retrieve patient information collected by different sources from the data’s final resting point in an EHR/EMR.
Interoperability opens the door to integration between systems, applications, and devices, unlocking vast value-generating potential for healthcare providers. HIEs permit these value-generating healthcare data sets to be securely accessed through Application Programming Interfaces (API). REST, SOAP, and SMTP APIs enable the pulling of patient data from clinical data sources or repositories to deliver patient information to the healthcare destination requesting it.
The prospect of sharing health-related data naturally evokes concerns around security and patient privacy. Since the protection of sensitive patient health information is of the utmost importance within the healthcare industry, interoperability between HIE solutions hinges on compliance with healthcare regulatory standards such as HL7 and FHIR.
These concerns may be understandable but can easily be put to rest. Healthcare software developers with deep industry knowledge, are able to utilize privacy laws to ensure complete electronic compliance.
Terminology standards codify the semantics used in healthcare data sharing. These standards are created by stakeholders ranging from the American Medical Association (AMA) to the World Health Organization (WHO) and include terminology, structured vocabulary, code sets, and classification systems.
Patient data needs to be able to be both viewed and understood by healthcare professionals having data pulled. Regardless of the application or vendor, the Healthcare Information and Management Systems Society (HIMSS) requires that standards of use must be followed to ensure that data can not only be exchanged, but also presented in an understandable and accurate manner.
An extensive range of predefined HIE interface code standards must be followed during development, including LOINC, CPT, SNOMED, RxNorm, ICD-9, ICD-10, NDC, and other clinical coding standards that fall under HIPAA guidelines. Following these codes ensures uniform identification of clinical statements through medical code interpretation. With universally understood codes, diagnoses and procedures are recorded to develop insurance claims, helping to determine accurate copay amounts for patients.
HIEs rely on secure, encrypted, and reliable messaging to transfer patient information over the internet to other healthcare providers. For obvious reasons, the way data is presented can determine the kind of care a patient receives. If patient information is presented in a way that is unclear or confusing to medical professionals, the risk of improper treatment increases exponentially.
Further, full integration between clinical data systems also relies on architectures built using HTTP, FTP, MIME, or HISP messaging protocols. Additionally, an extensive range of predefined HIE interface messaging protocols and EDI tools must be adhered to, including CDA, CCD, X12, EDIFACT, and NCPDP. With these clinical data exchange standards implemented, EHRs are able to securely “push” data to the provider requesting it without the threat of data breaches.
There are three types of HIE architectures, with all three exchange models typically being used within healthcare systems to enable the best exchange architecture possible.
Directed exchanges are used to push information from one healthcare provider to another through secure electronic channels. Providers can push clinical information, medical encounter alerts, patient discharge information, test results, and more.
Query-based HIE exchanges allow providers to electronically request patient information from other providers through requests called “pulls.” This kind of exchange is most helpful in instances of emergency care or unplanned healthcare visits.
Consumer mediated exchanges allow patients to collect, manage, correct, and transfer their own personal health information. This data includes demographic, medical, and billing information which can all be sent to providers. In cases where a consumer accesses their own health information to find errors, this exchange method allows them to update any incorrect or inaccurate medical history.
HIEs can operate individually (for one healthcare organization only), regionally, or as a nexus of networks. These three levels usually interface with each other within any given market area.
Serving populations of patients, HIE networks generally consist of multiple independent HIEs. These networks tend to operate federally or at the state level and are usually government-funded and operated.
Regional exchanges improve a local area’s connectivity and care efficiency. Consisting of multiple health organizations within a specific area, they are usually governed by independent, nonprofit health information organizations. These exchanges can also be funded and operated by the government or various non-profit groups.
Regional exchanges can connect local public health organizations, hospitals, and physicians, as well as national groups like insurance providers for complete health information visibility.
Private or proprietary HIE exchanges are funded, operated, and used by private healthcare organizations. They integrate providers and patients within a given area and focus on improving the individual organization’s overall clinical performance.
The range of privacy laws regulating digital medical information exchange is difficult for individual practitioners and organizations to navigate all on their own. There’s also the need to ensure compatibility between disparate systems. With advanced HIE software solutions, healthcare organizations can not only securely transmit patient data but also enhance overall productivity and profitability.
HIEs aren’t only revolutionizing individual patient care. Currently, HIE integrated applications are being used to manage everything from entire clinic workflows to regional outbreaks.
With innovation in this sector is in its infancy, it’s not possible to predict what these applications will be capable of offering even within the next five years. One thing that is certain, though, is that these innovations will exponentially increase the value healthcare providers can deliver.
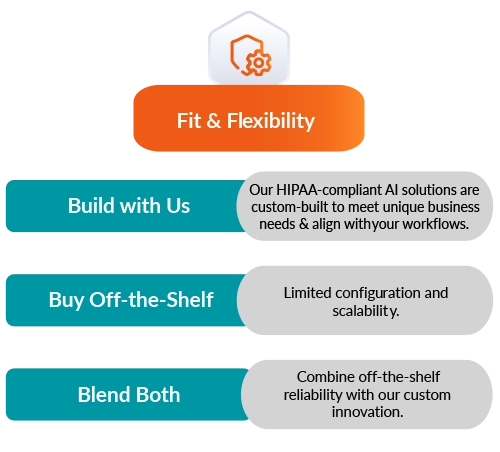
Speed, control, and scalability aren’t one-size-fits-all. Whether you're launching a new healthcare solution or upgrading legacy systems, this quick-hit comparison helps you weigh the trade-offs—custom builds, off-the-shelf ease, or a hybrid that delivers fast and flexibly.
Build with Us
Buy Off-the-Shelf
Blend Both
Speed to Value
We build from the ground up around your workflows.
Fast deployment with minimal setup.
Hybrid rollout with a rapid MVP delivery
Fit & Flexibility
Our HIPAA-compliant Al solutions are custom-built to meet unique business needs & align with your workflows.
Limited configuration and scalability.
Combine off-the-shelf reliability with our custom innovation.
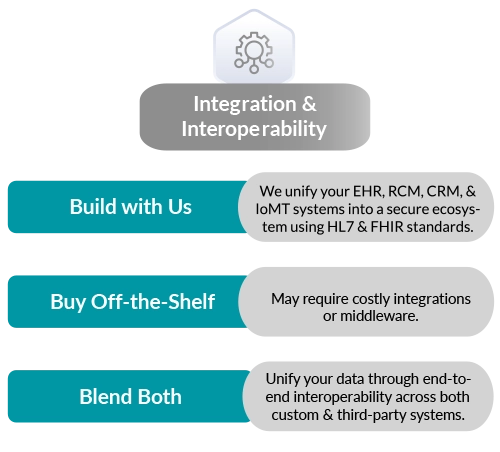
Integration & Interoperability
We unify your EHR, RCM, CRM, & JoMT systems into a secure ecosys-tem using HL7 & FHIR standards.
May require costly integra-tions or middleware.
Unify your data through end-to-end interoperability across both custom & third party systems.
Ownership & Scalability
You own the code, the IP, and the roadmap - built for long-term growth.
Vendor-controlled roadmap and licensing.
Shared scalability with flexible expansion options.


Disclaimer:
This content has been made available for information purposes only. Views and opinions expressed in this content are those of the individual author only and do not necessarily represent the opinions and views of Chetu. Chetu, and its representatives, make no representation or warranty of any kind, express or implied, regarding the accuracy, adequacy, validity, reliability, availability, or completeness of any information of this content. Under no circumstances shall Chetu, or its representatives, have any liability to you or any loss or damage of any kind incurred as a result of the use of this content or reliance on any information provided in this content. Your use of this website and your reliance on any information on this content is solely at your own risk.
About Chetu:
Founded in 2000, Chetu empowers businesses with AI and digital transformation solutions, supporting startups, SMBs, and Fortune 5000 companies. We deliver end-to-end software solutions backed by global digital intelligence and industry expertise. Our customized software delivery model and one-stop-shop approach span the full technology spectrum. Headquartered in Sunrise, Florida, Chetu operates 13 locations across the U.S., Europe, and Asia.
See more at: Chetu Blogs
Privacy Policy | Legal Policy | Careers | Sitemap | Referral | Contact Us
Copyright © 2000- 2026 Chetu Inc. All Rights Reserved.



